
Have you ever wondered if palliative care is all about saying final goodbyes to your sick loved ones? Well, guess what – it’s not. Palliative care is so much more than that.
Palliative care is like a helping hand for people dealing with serious illnesses, making life better, not worse. This article will help you see what palliative care is really about, why it’s important, and how it can make things easier for those who need it. So, whether your loved ones are struggling with a serious disease, or you’re just curious and want to understand palliative care better, keep reading. We’re here to keep it simple and clear for you.
What Does Palliative Care Mean?

Palliative care is a holistic approach to medical treatment with a focus on improving the quality of life for individuals facing serious illnesses. This form of care is not limited to end-of-life situations and can be integrated at any stage of a serious disease or chronic illness.
Palliative care aims to provide relief from the symptoms and stress of a serious illness. It focuses on improving the patient’s and their family’s quality of life by addressing physical, emotional, and spiritual needs.
What is the role of palliative care in improving quality of life?
The primary role of palliative treatment is to enhance the overall well-being of patients dealing with serious illnesses. It involves managing their pain through medication and better nutritional support, addressing their emotional and psychological distress, and supporting them in making informed decisions about their treatment options.
Who provides palliative care?
Palliative care is basically teamwork involving a group of various healthcare professionals. This multidisciplinary team may include doctors, nurses, social workers, caregivers, chaplains, and other specialists who work together to address the diverse needs of patients and their families.
When should palliative care be considered?
Palliative care should be considered at any point in a serious illness, regardless of the prognosis. It is not reserved for end-of-life situations but can be integrated alongside curative treatments to provide comprehensive support and symptom management.
Differentiating palliative care from hospice care
While palliative care and hospice care share similarities, they differ in their scope and timing. Palliative care is applicable at any point of a chronic illness, whereas hospice care caters to patients in their final days of life. Understanding this distinction is crucial for making informed decisions about the type of care that best suits the patient’s needs.

Debunking 8 Palliative Care Myths And Misconceptions
Certainly, palliative care is an important component of healthcare that focuses on improving the quality of life for patients facing serious illnesses. However, palliative care is often misunderstood, and this misunderstanding can lead to unnecessary fear and anxiety.
Let’s explore and debunk some common myths associated with palliative care.

Does Palliative Care Mean Death?
Myth: Palliative care equals the end of life.
Debunked: Palliative care is not synonymous with death. It is also not reserved for just dying patients. It is about enhancing the overall well-being of patients facing serious illnesses, regardless of their life expectancy. Palliative care provides physical, emotional, and spiritual support to improve the patient’s quality of life throughout their illness journey.
Is Palliative Care Only For Terminal Cancer Patients?
Myth: Palliative care is exclusively for those with terminal cancer.
Debunked: Palliative care is not limited to cancer or any other terminal illnesses. It applies to a broad range of serious medical conditions, such as heart failure, chronic obstructive pulmonary disease (COPD), kidney failure, Alzheimer’s, and other chronic neurological disorders. Palliative care can be beneficial at any stage of an illness, not just in the final moments.
Is Palliative Care All About Painkillers?
Myth: Palliative care revolves around pain relief through medications.
Debunked: While pain management is a crucial component of palliative care, it is not the sole focus. Palliative care addresses various aspects of a patient’s well-being, including emotional and spiritual needs. It emphasizes a holistic approach, incorporating medications, counseling, and other supportive measures to enhance the overall quality of life.
Does Treatment End Where Palliative Care Starts?
Myth: Palliative care means the end of medical treatment.
Debunked: Palliative care works alongside curative treatments. Patients can receive palliative care simultaneously with other medical interventions aimed at treating their illness. It complements other medical approaches by focusing on symptom management and improving the patient’s overall comfort.
Do Patients In Palliative Care Who Stop Eating Die Of Starvation?
Myth: Patients in palliative care, if they stop eating, will die of starvation.
Debunked: In palliative care, the emphasis is on comfort and dignity. While changes in appetite are common in serious illnesses, palliative care teams work to address these issues and find alternative ways to fulfill their nutritional needs.
Nutritional support, counseling, and other interventions are taken to ensure patients receive the care they need, even if their eating patterns change. A patient may die of their illness, but not starvation.
Is Palliative Care The Same As Hospice Care?
Myth: Palliative care and hospice care are interchangeable terms.
Debunked: Palliative care and hospice care share similarities, but they are distinct. Palliative care is applicable at any stage of a serious illness and can be provided alongside curative treatments. Hospice care, on the other hand, is specifically for patients nearing the end of life and forgoes curative treatments in favor of comfort-focused care.
Is Palliative Care The Same As Euthanasia/Assisted Suicide?
Myth: Palliative care involves euthanasia or assisted suicide.
Debunked: Palliative care is centered on providing comfort, support, and symptom management. It does not involve hastening death. Euthanasia or assisted suicide is an entirely different practice that involves deliberate actions to end a patient’s life, often in response to severe, incurable suffering. These practices are subject to complex ethical and legal considerations and are contrary to the goals of palliative care.
Is Palliative Care Only Provided In Hospitals?
Myth: Palliative care is only delivered in hospital settings.
Debunked: Palliative care can be administered in various settings, including hospitals, nursing homes, assisted living facilities, and even at home. The goal is to provide personalized care where the patient feels most comfortable. Home-based palliative care is increasingly common, allowing patients to receive support in familiar surroundings.
Palliative Care Support Services
The comprehensive support system of palliative care involves a dedicated palliative care team, a wide range of services, and a holistic approach that considers emotional and spiritual well-being.

The Palliative Care Team
A key aspect of palliative care is the collaborative effort of a specialized team. This multidisciplinary team typically includes doctors, nurses, physiotherapists, counselors, social workers, carers, and other healthcare professionals working together to address the diverse needs of patients.
Each member contributes their unique expertise to create a tailored care plan that considers the physical, emotional, and spiritual aspects of the patient’s well-being.
Range Of Services Provided In Palliative Care
Palliative care is like a toolbox with many tools to help with different challenges. One important tool is managing pain and symptoms, using medicines or other ways to make the person feel better.
Another tool is organizing care – making sure everyone involved in treatment collaborates. They also help with planning for the future, so the patient’s wishes are followed.
Palliative Care For Different Conditions
Palliative care is not limited to specific terminal diseases or conditions; it applies to a wide range of illnesses, including but not limited to cancer, heart failure, chronic obstructive pulmonary disease (COPD), Alzheimer’s, Parkinsonism, kidney failure, and neurodegenerative disorders.
The focus is on alleviating suffering and enhancing the well-being of patients, regardless of the prognosis. Palliative care can be introduced at any stage of a serious illness, working alongside curative treatments to provide a holistic approach to care.
How Palliative Care Supports The Emotional Well-Being Of Patients And Families
Dealing with a serious illness can be emotionally challenging for both patients and their families. Palliative care recognizes the importance of addressing the emotional and psychological burden of the journey.
The team provides counseling and other resources to help patients and their families cope with the impact of the illness. By fostering open communication and creating a supportive environment, palliative care enhances the emotional well-being of patients and their loved ones.

Importance Of Spiritual Support In Palliative Care
Recognizing the significance of spirituality in the healing process, palliative care often includes spiritual support as a vital component. Chaplains or spiritual counselors work with patients to provide comfort, guidance, and assistance in finding meaning and purpose during challenging times. This aspect of palliative care respects the diverse spiritual and cultural beliefs of patients, fostering an inclusive and compassionate approach to holistic well-being.
Comprehensive Plan of Care
One of the essential aspects of palliative care is facilitating open and honest discussions about end-of-life wishes. These conversations may be challenging, but they are crucial for ensuring that patients receive the care they truly want and deserve. By involving loved ones in these discussions, patients can create a comprehensive care plan that aligns with their values and preferences.
It’s important to understand that palliative care isn’t merely about end-of-life care; it’s about improving the overall well-being of patients and their families throughout the entire journey of any serious illness. Integrating palliative care into the broader spectrum of healthcare services ensures that patients receive holistic and compassionate support as they navigate their medical conditions, enhancing the quality of life during a challenging time.
How To Access Palliative Care For Your Elderly

Are you looking to hire palliative care for your elderly loved ones? If yes, we’ve discussed here a few steps to get palliative care.
How To Find Palliative Care Services In Your Area
Finding palliative care services in your area is the first step in ensuring your elderly loved one receives the care they need. Here’s what you need to do:
- Start by discussing your elderly family member’s condition with their primary healthcare provider. They can often recommend palliative care services or specialists in your area.
- Use the internet to search for palliative care providers near you. Many hospitals, healthcare organizations, and senior care facilities have websites with directories of palliative care services.
- Reach out to friends, family, or support groups who may have experience with palliative care. They can provide valuable insights and recommendations based on their own experiences.
- Hospice care facilities often provide palliative care services. Get in touch with your local hospice to inquire about available options and resources.
- Hospital or healthcare facility social workers can be a great resource. They can guide you in finding appropriate palliative care services and help you navigate any financial aspects.
Understanding The Financial Aspects Of Palliative Care
Palliative care can be costly, but it’s essential to ensure your loved one’s comfort and well-being. Here’s how to understand the financial aspects:
- Review your elderly family member’s insurance policies, including Medicare or Medicaid, to see what palliative care services may be covered.
- Have open and honest discussions with palliative care providers about the expected costs. They may offer financial assistance or payment plans.
- Some nonprofit organizations and charities provide financial assistance for palliative care. Look into these options to ease the financial burden.
- Consider creating an advanced care plan with your loved one. This can help allocate resources and ensure their wishes for palliative care are met without unnecessary financial strain.

Exploring Home-Based Palliative Care Options
Home-based palliative care can be a viable option for your elderly family member. Here’s what you need to know:
- Palliative care providers will assess your home to ensure it meets the requirements for safe care delivery.
- Care plans are personalized to your loved one’s needs and preferences, allowing them to receive care in the comfort of their own home.
- Home-based palliative care encourages family involvement and support, fostering a more nurturing environment for your elderly family member.
- Palliative care teams can work with home health agencies to coordinate services, making it easier for your loved one to receive comprehensive care.
Benefits Of Integrating Palliative Care Into Care Facilities
Integrating palliative care into senior care facilities ensures that the elderly receive the comfort, relief, and privacy they need during challenging times.
- Patients in care facilities can benefit from the expertise of palliative care teams, leading to improved symptom management and emotional support.
- Integration facilitates better communication between care facility staff and palliative care specialists, ensuring a cohesive approach to patient care.
- Patients who receive palliative care while in a care facility may experience fewer readmissions, leading to better overall outcomes.
- Families can also benefit from integrated care by having access to palliative care services during their loved one’s stay in the care facility.
The Future Of Palliative Care
Palliative care is entering a new phase with exciting changes and improved ways of helping patients. Here’s a look at the latest trends and changes in this important area of healthcare.
Advancements in Palliative Care in the USA
Palliative care in the USA is increasingly focusing on a holistic approach, addressing not just physical but also emotional, social, and spiritual aspects of patient well-being. This involves a multidisciplinary team of healthcare professionals, including physicians, nurses, and social workers, to ensure comprehensive support.
Innovations in care include advancements in pain management, using targeted medications and techniques like nerve blocks and acupuncture, as well as the integration of complementary therapies such as music and art therapy.
Policy Changes and Access to Palliative Care
Recent policy changes have significantly impacted access to palliative care in the USA. According to the Affordable Care Act, the expansion of Medicaid has resulted in higher palliative care use, especially among advanced cancer patients.
This expansion has particularly benefitted patients in states that adopted it, indicating that policy changes can substantially improve access to palliative care services. Additionally, state-level initiatives are focusing on broadening access to palliative care, with a special emphasis on home-based care.
Palliative Care In Assisted Living Homes
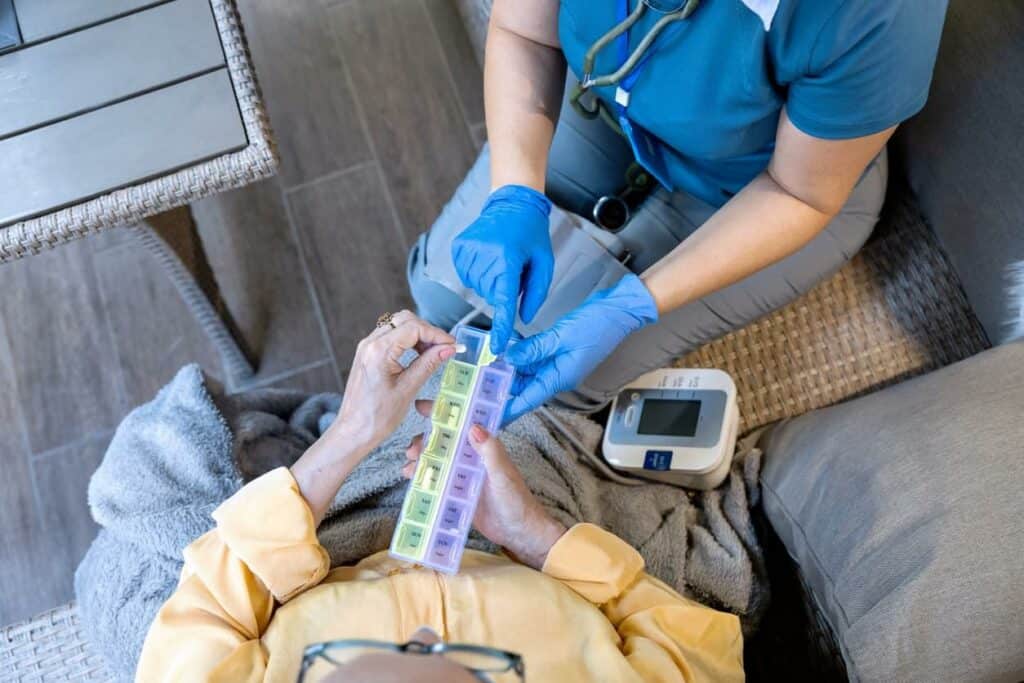
Palliative care in assisted living homes like Amy’s Eden is a compassionate approach to care that focuses on enhancing the quality of life for senior residents with serious illnesses. Unlike hospitals or specialized palliative care centers, assisted living facilities offer a unique blend of support that balances medical needs with a comfortable, home-like environment.
In these settings, palliative care is tailored to each person’s needs, emphasizing not just physical comfort, but also attending to emotional, social, and spiritual well-being. This holistic approach ensures that residents receive comprehensive care that respects their dignity and personal preferences.
Alongside this, emotional and spiritual support is offered through counseling and various activities that promote a sense of community and belonging. Family members are also encouraged to be involved in the care process, providing a familiar and comforting presence for the resident.
This supportive environment in assisted living homes makes it an ideal setting for palliative care, where the focus is on enhancing the quality of life and providing care with compassion and respect.
Conclusion
Now you know how palliative care is not just for the end of life. It’s a caring support for anyone with serious illnesses. It helps with pain, comfort, and emotional support, making life better for patients and their families. Remember, palliative care is about improving the quality of life at any stage of illness, not just the end.
For those seeking such compassionate care for their loved ones in a home-like setting, Amy’s Eden offers this kind of care in a warm, home-like setting. It’s a place where seniors get personalized care that looks after their medical, emotional, and spiritual needs.
Here, we treat every resident with dignity and respect, making their days more comfortable and meaningful. Contact us today to learn more about our palliative care services.
